NJMS Curriculum at a Glance
The New Jersey Medical School curriculum is the product of extensive discussion and faculty/student collaboration involving basic science and clinical departments.
The Curriculum Framework Model is comprised of 3 main phases and is based on the following guiding principles and key priorities:
- Service Learning
- Longitudinal clinical experiences
- Basic science integration into clerkship years
- Integrated organ systems-based curriculum with capstones
- Interprofessional educational opportunities
- Active learning
- Milestone assessments and monitoring of curriculum
- Expanded elective opportunities early in curriculum
- Student Wellness
The Curriculum below is effective for the Class of 2030, starting in July 2026.
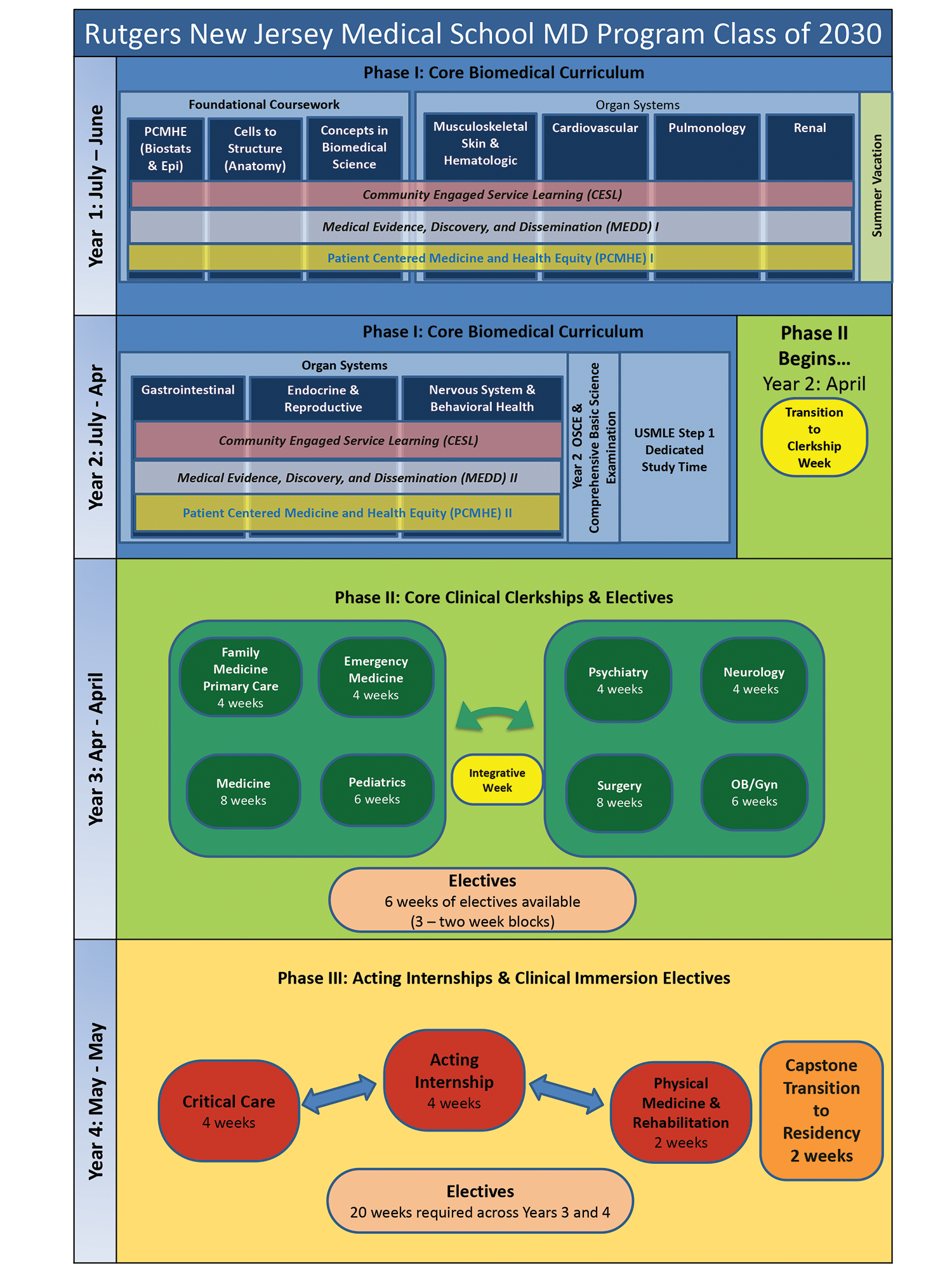
Click here to enlarge
The main curriculum is visualized as "Blocks" where each section is taught with an integrated organ systems approach (for example the cardiovascular organ block), there are certain key aspects of the curriculum that exist across and throughout the curriculum. These are described as "Threads".
For example, Pediatrics and Geriatrics is an important thread such that when an organ system is being taught, (e.g. pulmonary), both pediatric (e.g. cystic fibrosis) and geriatric (e.g. lung cancer) conditions are emphasized.
Phase 1
Core Biomedical Curriculum builds on the foundational principles and provides an in-depth study of structure, function, and disease in an integrated organ system-based approach. These integrated courses will be co-led by basic science and clinical faculty.
Patient Centered Medicine and Health Equity (PCMHE) provides the skills set to integrate medical knowledge with expert communication skills, clinical acumen, empathy, and a commitment to enhancing opportunities for health and wellness for our patients and our communities. *PCMHE is the previously named Healing, Humanism, and Health Equity (HHH) course and will be implemented in 2025-26 for the incoming Class of 2029.
Phase 2
Phase 2 begins in the third year with core clerkship experiences. One of the major goals is to provide expanded early elective opportunities. This additional time for electives in Phase 2 is consistent with the primary aim of emphasizing both individualization and standardization in the curriculum. A key element will be flexibility, allowing students to pursue electives and wellness opportunities. Careful attention is paid to mapping clinical experiences, achievement of milestones and greater basic science integration.
There is a commitment to build in the thread of basic foundational science concepts into Phase 2 through structured learning activities within the clerkships, including applications of such concepts as anti-microbial resistance, and clinical pharmacology.
Phase 3
Phase 3 allows for ample elective time and further career exploration and differentiation. There will be required acting-internships and elective time with an effort to emphasize certain foundational science topics relevant to the emergently and critically ill patient.
Elective time is major feature of Phase 3 in addition to a transition to residency capstone course that will help students in preparation for residency.

