Overview
Our curriculum continues to evolve as we identify innovative pathways to enhance academic growth and strenghten the clinical experience. Most recently we have added a community-ED rotation (at Cooperman Barnabas Medical Center in Livingston, NJ) as well as expanded our offerings in sub-specialty areas as we focus on training the next generation of emergency physicians in innovative and effective ways. The outline below reflects the curriculum as it was implemented in July 2025 for our incoming class of 2029. Minor variations exist for residents that have already begun training.
Each of our four years is divided into thirteen, four-week rotation blocks as follows (rotations do not occur in the sequence below).
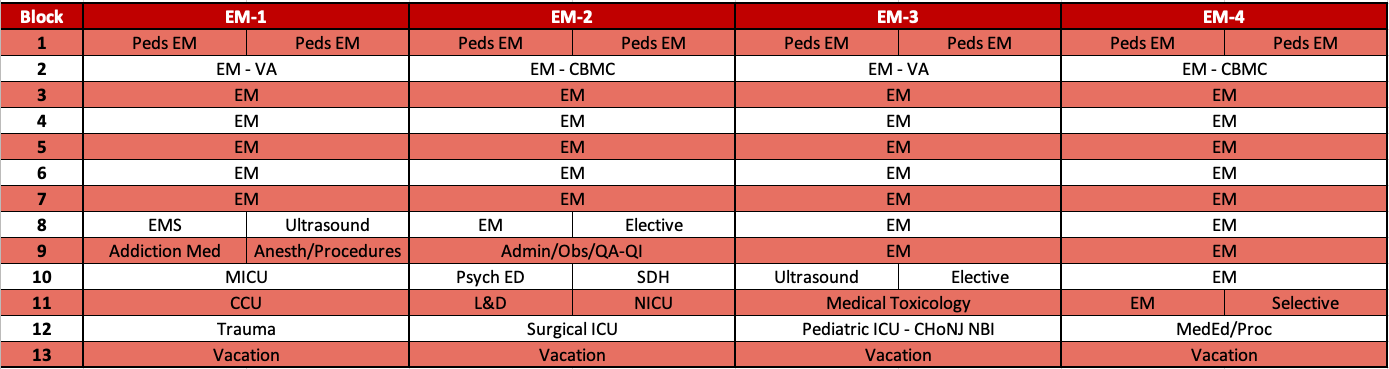
All EM blocks include approximately 10% Pediatric ED shifts and daily exposure to Psychiatric ED patients

